Hip injuries are extremely common in people of all ages. Individuals who participate in sports have an increased risk of hip injuries. Seniors and people carrying extra weight also are at risk for hip injury.
HIP

Hip Physical Therapy
Questions & Answers
Hip Osteoarthritis
Hip osteoarthritis is a common type of osteoarthritis (OA) that breaks down the cartilage in the hip joint. Since the hip is a weight-bearing joint, osteoarthritis can cause significant problems. Hip osteoarthritis is caused by deterioration of articular cartilage and wear-and-tear of the hip joint. Hip OA is a degenerative joint disease involving cartilage of the hip and inflammation of the soft tissue linings. Osteoarthritis may be diagnosed by your history and physical examination or by an X-ray. An X-ray may not be helpful since early stages of arthritis may not be seen on X-ray while moderate to advanced stages of arthritis are recognizable on physical exam.
Hip Tumors
Congenital Dysplasia/Antiverzion
Congenital Dysplasia of the hip joint is a condition that results in the deformation, and possible chronic dislocation of the hip joint. The hip joint becomes deformed, leading to an unstable joint. Congenital Dysplasia starts at birth, but is an ongoing process, most detectable in adults. At birth, or soon after, children may appear to have perfectly normal hip joints, but later on in life, suffer from severe Congenital Dysplasia. The troublesome joint is usually replaced with artificial prosthesis. Although Congenital Dysplasia can occur in men, it is more common in women. It has been noticed that about one man to every nine women acquire Congenital Dysplasia.
Symptoms:
- Legs of different lengths.
- Uneven thigh skin folds.
- Less mobility or flexibility on one side.
Hip Fractures
You can break your hip at any age, but the great majority of hip fractures occur in people older than 65. As you age, your bones slowly lose minerals and become less dense. Gradual loss of density weakens bones and makes them more susceptible to a hip fracture.
A hip fracture is a serious injury, particularly if you’re older, and complications can be life-threatening. Fortunately, surgery to repair a hip fracture is usually very effective, although recovery often requires time and patience.

Symptoms:
- Immobility immediately after a fall
- Severe pain in your hip or groin
- Inability to put weight on your leg on the side of your injured hip
- Stiffness, bruising and swelling in and around your hip area
- Shorter leg on the side of your injured hip
- Turning outward of your leg on the side of your injured hip
Hip Dislocations
A hip dislocation occurs when the head of the thighbone (femur) slips out of its socket in the hip bone (pelvis). In approximately 90% of patients, the thighbone is pushed out of its socket in a backward direction (posterior dislocation). This leaves the hip in a fixed position, bent and twisted in toward the middle of the body. The thighbone can also slip out of its socket in a forward direction (anterior dislocation). If this occurs, the hip will be bent only slightly, and the leg will twist out and away from the middle of the body.
A hip dislocation is very painful. Patients are unable to move the leg, and if there is nerve damage, they may not have any feeling in the foot or ankle area.

Symptoms:
- Swelling
- Hip/ Knee pain
- Hip stiffness
- Difficulty walking
- Numbness/ weakness
- Immobility
- Deformed hip and/or leg
Hip Pointers
A hip pointer injury is an extremely painful, acute injury to the iliac crest of the pelvis. The injury causes bleeding into the abdominal muscles, which attach to the iliac crest. The bone and overlying muscle are often bruised, and the pain can be intense. Pain may be felt when walking, laughing, coughing, or even breathing deeply.
Hip pointers are the result of a direct blow to the iliac crest, whether from a direct hit from a helmet, or a hard fall. Hip pointers are common in contact sports, such as football and soccer.
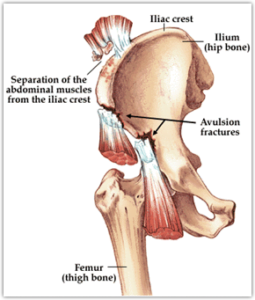
Symptoms:
- Extreme pain over the iliac crest
- Bruising
- Hematoma
- Muscle spasm
Labral Tears
The labrum is a type of cartilage that surrounds the socket of ball-and-socket joints. A labrum is found in both the shoulder and the hip joint. The labrum forms a ring around the edge of the bony socket of the joint. It helps to provide stability to the joint by deepening the socket, yet unlike a bone, it also allows flexibility and motion.

Symptoms:
- Groin pain
- Clicking and snapping sensations in the hip
- Limited motion of the hip joint
Tendonitis/Strains (Repetitive Injury)
Hip Tendonitis is often experienced by individuals who do repetitive movements that involve the soft tissues that surround the hip. Their frequent gestures usually result to pain and weakness in the hip region.
The hip, or the greater trochanter, is considered as the bony bulge of the femur and layers of fat and muscle. The hip joint, which lies between the pelvis’s acetabulum and the femur, supports the mass of the whole body in standing, running or walking postures. The tendons and muscles around the hip are very powerful because they create great forces. This is also the reason why it is prone to tendon inflammation and muscle irritation.
Symptoms:
- Weakness over the hip tendon
- Acute pain hip tendons and muscles are moved
- Difficulty bending hips
- Thigh and hip swelling
- Infection and frequent fever
- Warmth, redness in the hips and thighs.
Hip Bursitis (Repetitive Injury)
Hip bursitis is swelling and pain of a bursa in your hip. A bursa is a fluid-filled sac that acts as a cushion or shock absorber between a tendon and a bone. A tendon is a cord of tough tissue that connects muscles to bones. Normally a bursa has a small amount of fluid in it. When injured, the bursa becomes inflamed. There are different types of hip bursitis. These types include trochanteric bursitis and ischial bursitis. Ischial bursitis causes pain at the base of the hips where you sit down. The amount of time that you have bursitis depends on the cause of bursitis. With treatment, many people feel better in about six weeks, but it may take longer for bursitis to heal.
Symptoms:
- Pain over the outside of your hip and thigh
- Pain moving from the buttock into the hip
- Pain in one side of the groin with slight pain in the opposite hip
- Stiff hip
- “Pop” or “snap” sound as leg flexes
- Difficulty climbing stairs
We’ve got answers to your questions. Click on the “v” next to each heading to learn more.
